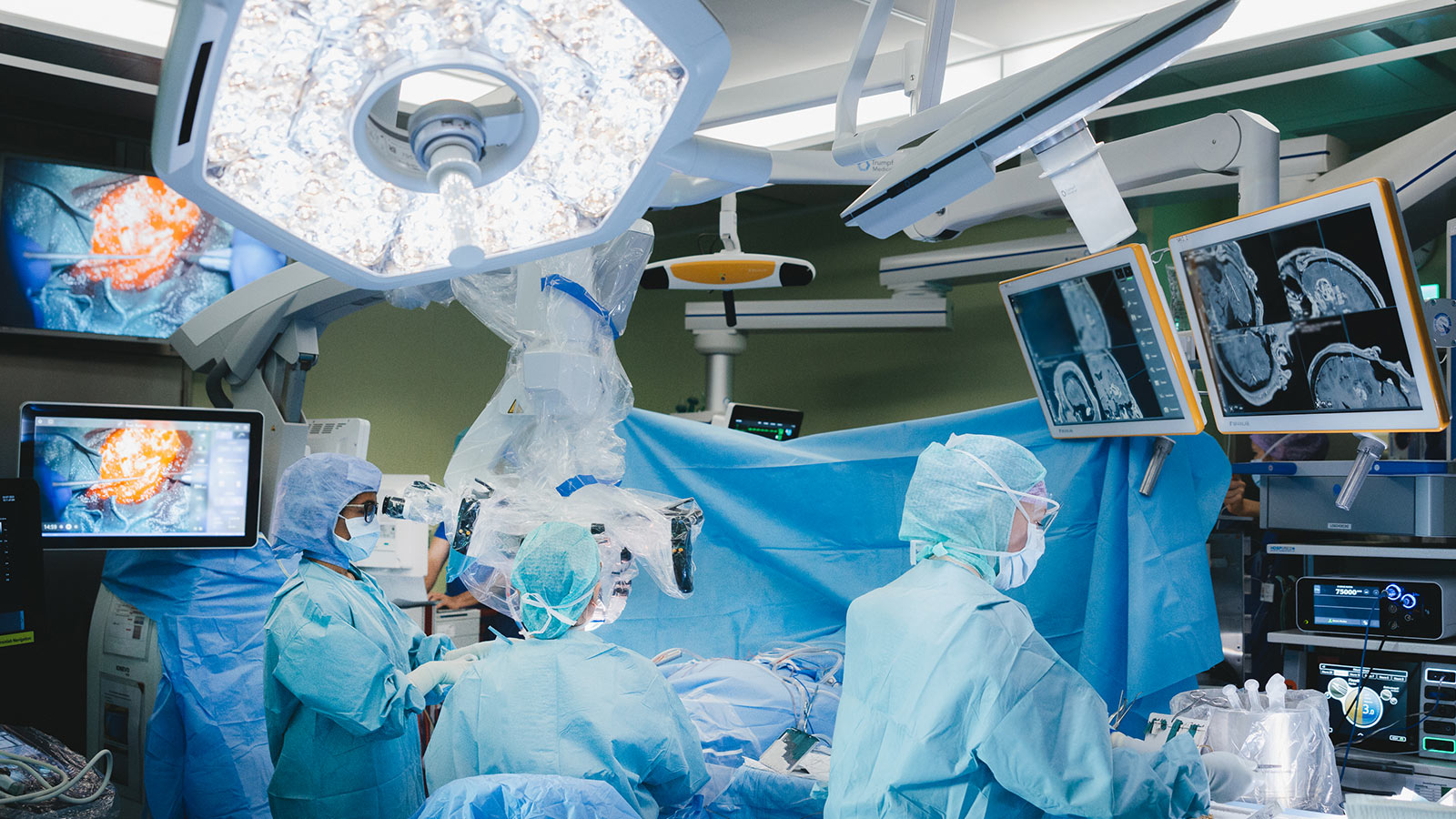
The research of today lays the foundation for the medicine of tomorrow. Every breakthrough brings us one step closer to safer surgeries and new, improved treatment approaches for previously incurable diseases. That is why research is so essential to our work.
Would you like to be part of this important mission and support us with your donation? Your contribution to neurosurgical research helps us advance our projects and give patients new hope. Together, we can shape the future of medicine and improve the chances of healing.
Neurosurgical research – Brain tumors
A key focus of our neurosurgical research is brain tumor research. It enhances safety and precision in procedures on the brain and spinal cord. With state-of-the-art technologies, we can visualize vital brain structures, making even the most complex procedures safer.
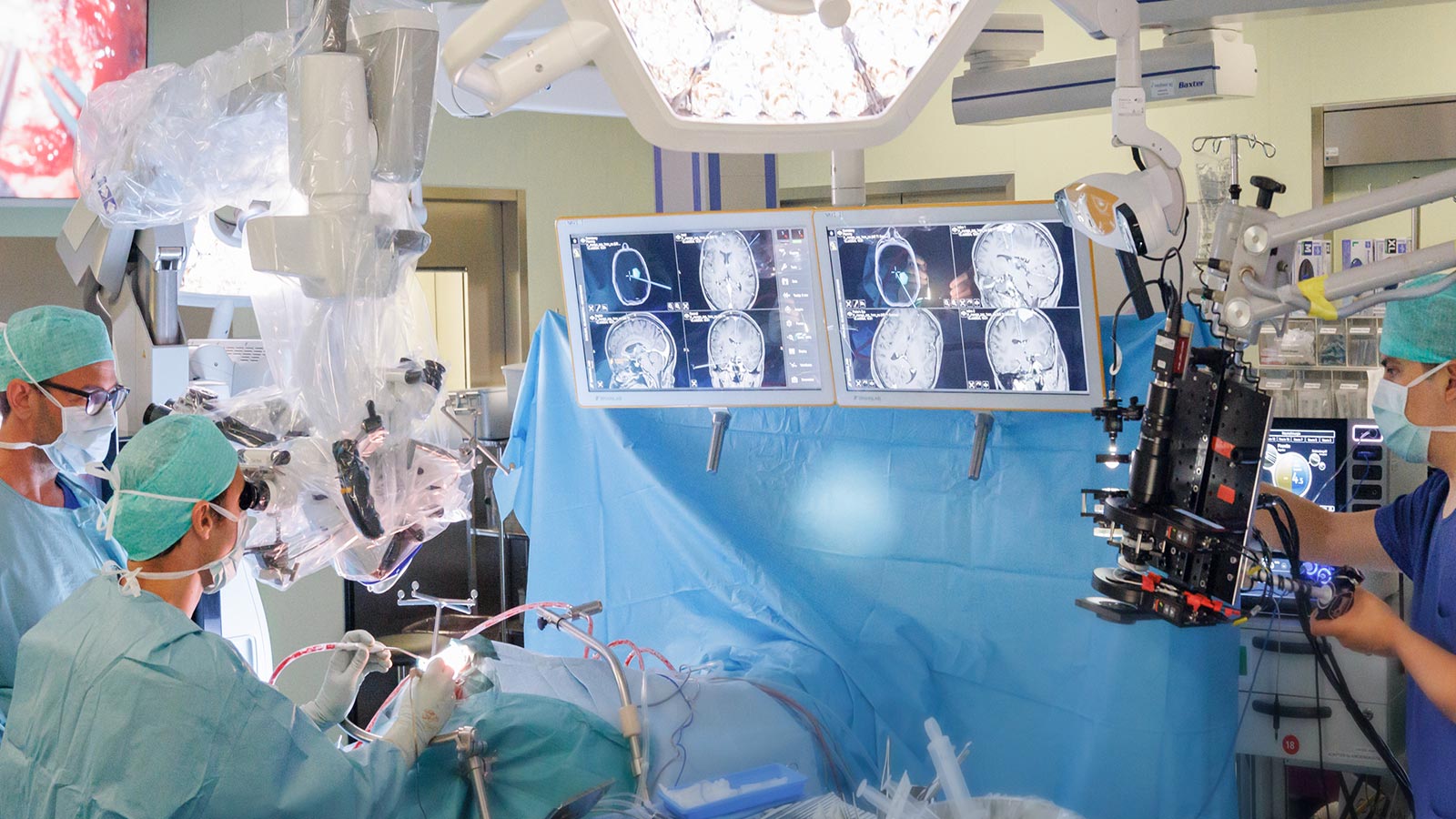
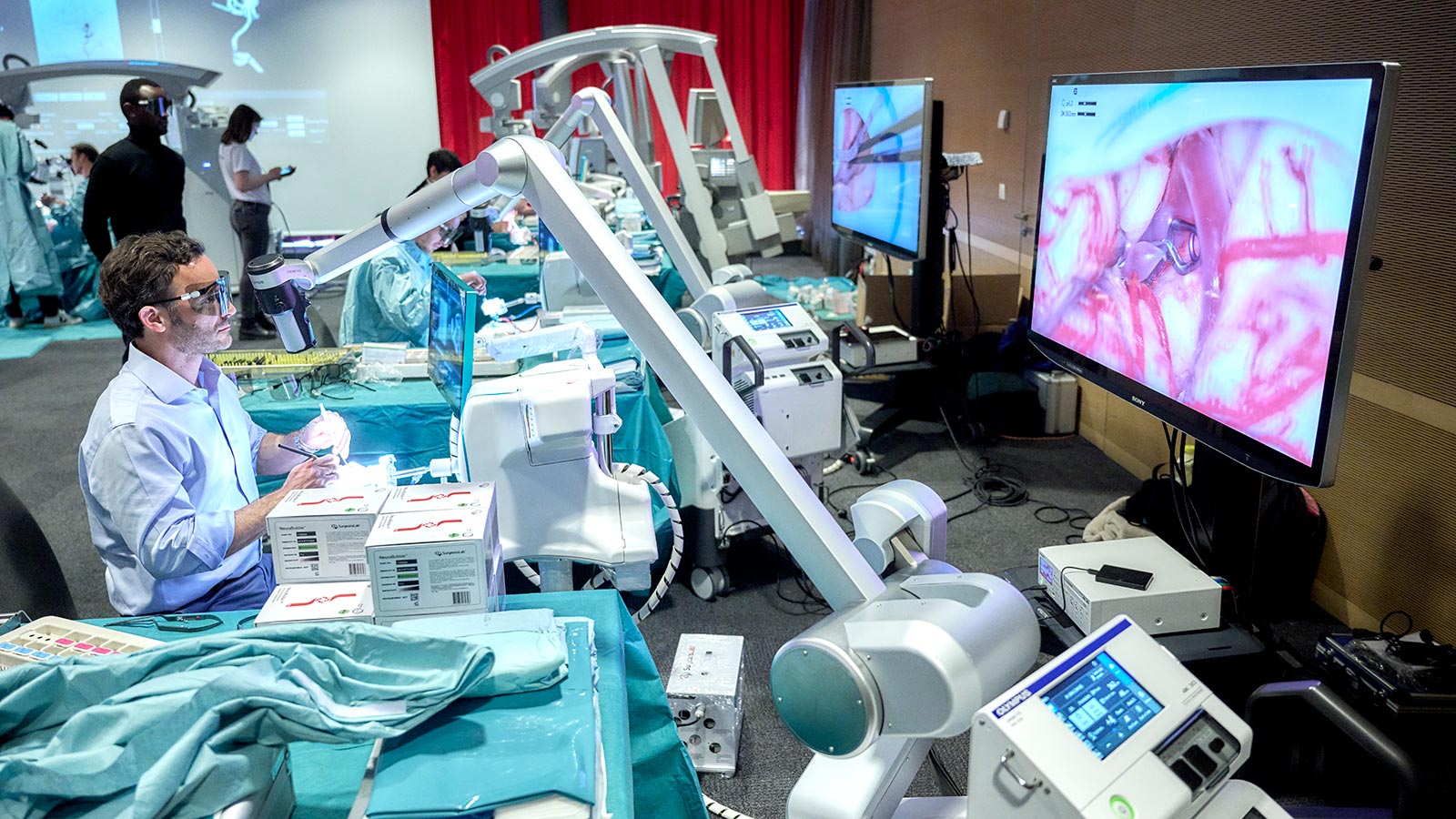
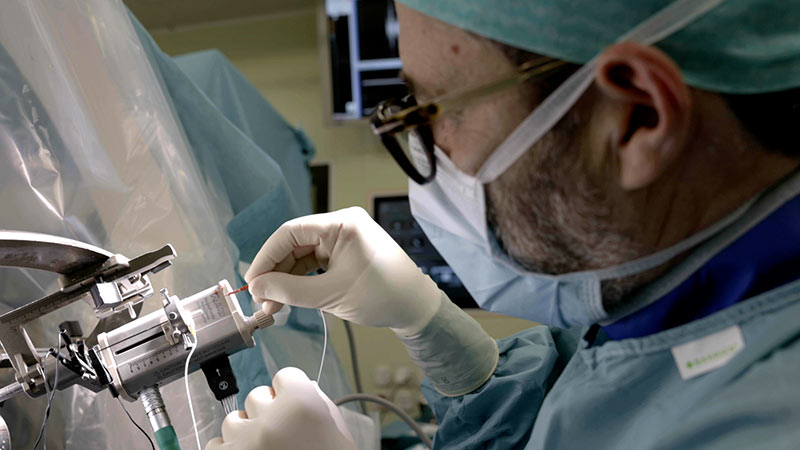
HORAO project: safer brain tumor surgeries
Support our major research project HORAO. We are working intensively on the development of a new surgical microscope that will enable more precise and at the same time gentler removal of brain tumors. The first prototypes are currently being tested in the OR.
Cerebrovascular research
Research in the field of vascular neurosurgery is crucial to continuously improve the treatment of life-threatening vascular diseases such as aneurysms, strokes, and vascular malformations, and to minimize risks for patients.
Research in functional neurosurgery
Millions of people worldwide suffer from diseases such as Parkinson's, epilepsy, or migraine, which are caused by malfunctions of the nervous system. Advances in research are enabling new therapies and better diagnoses, allowing those affected to lead more active and pain-free lives.