A herniated disc is a common condition that affects about 5% of people at some point in their lives. It is usually caused by age-related wear and tear of the spine, which begins as early as young adulthood. This can cause material from the disc to leak into the spinal canal, where it compresses nerves or the spinal cord. Typical symptoms include back pain as well as radiating pain, numbness, or weakness in the arms or legs.
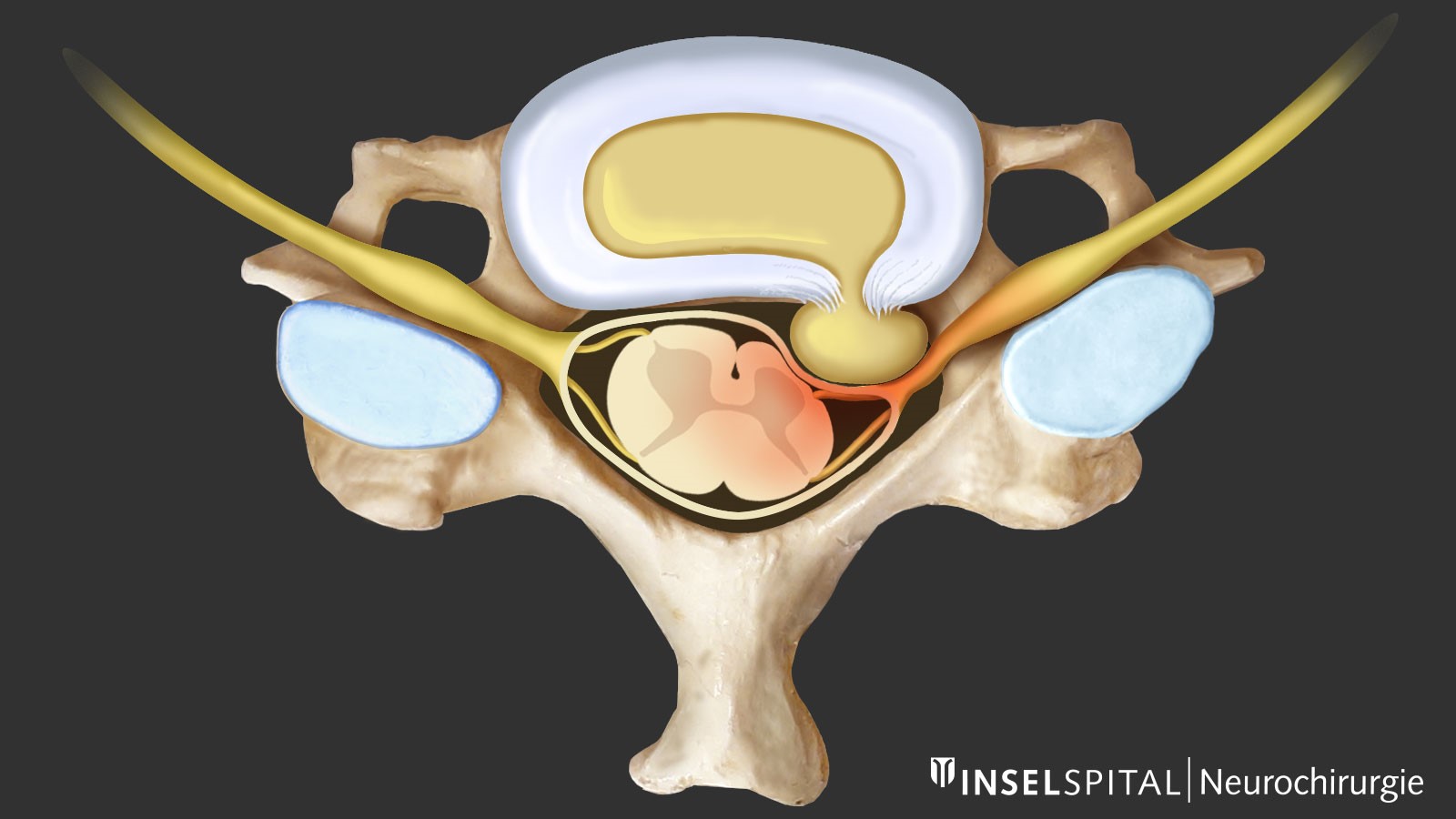
Is a herniated disc a a common public health condition?
The mobility of the spine comes at a price: As we age, natural signs of wear and tear occur:
- degeneration of the intervertebral discs
- loosening of ligaments
- bone changes
These processes begin as early as young adulthood and can be accelerated by repetitive strain, poor posture when lifting, and other factors. Several studies have also demonstrated a genetic predisposition to faster degeneration of the intervertebral discs.
Changes in the intervertebral discs are often detectable on imaging, but frequently cause no symptoms. A clinically significant herniated disc occurs much less frequently and affects about 5% of people over the course of their lives.
What is the function of the intervertebral disc?
The intervertebral disc is a cartilaginous disc between two adjacent vertebrae and serves as a shock absorber and hinge.
Humans have 23 intervertebral discs, from the second cervical vertebra to the coccyx. It is only because of these discs that the spine can move so flexibly.
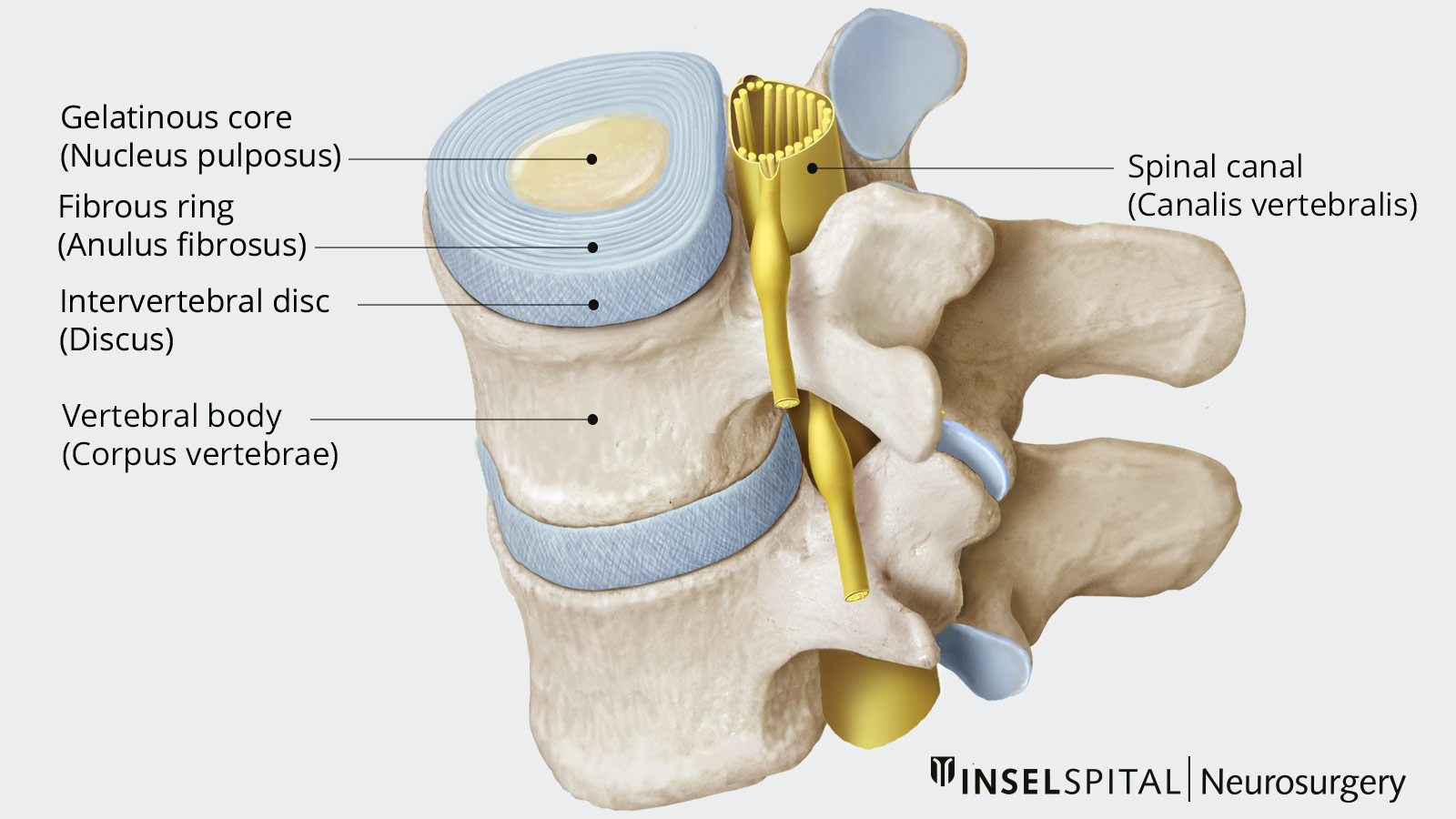
An intervertebral disc consists of three parts:
- a gelatinous inner core (nucleus pulposus)
- a strong outer fibrous cartilage ring (annulus fibrosus) and
- cartilaginous portions at the upper and lower ends that merge into the vertebral bodies
The intervertebral disc distributes the weight bearing down on the individual vertebral bodies evenly from the upper to the lower vertebral body.
What happens during a herniated disc?
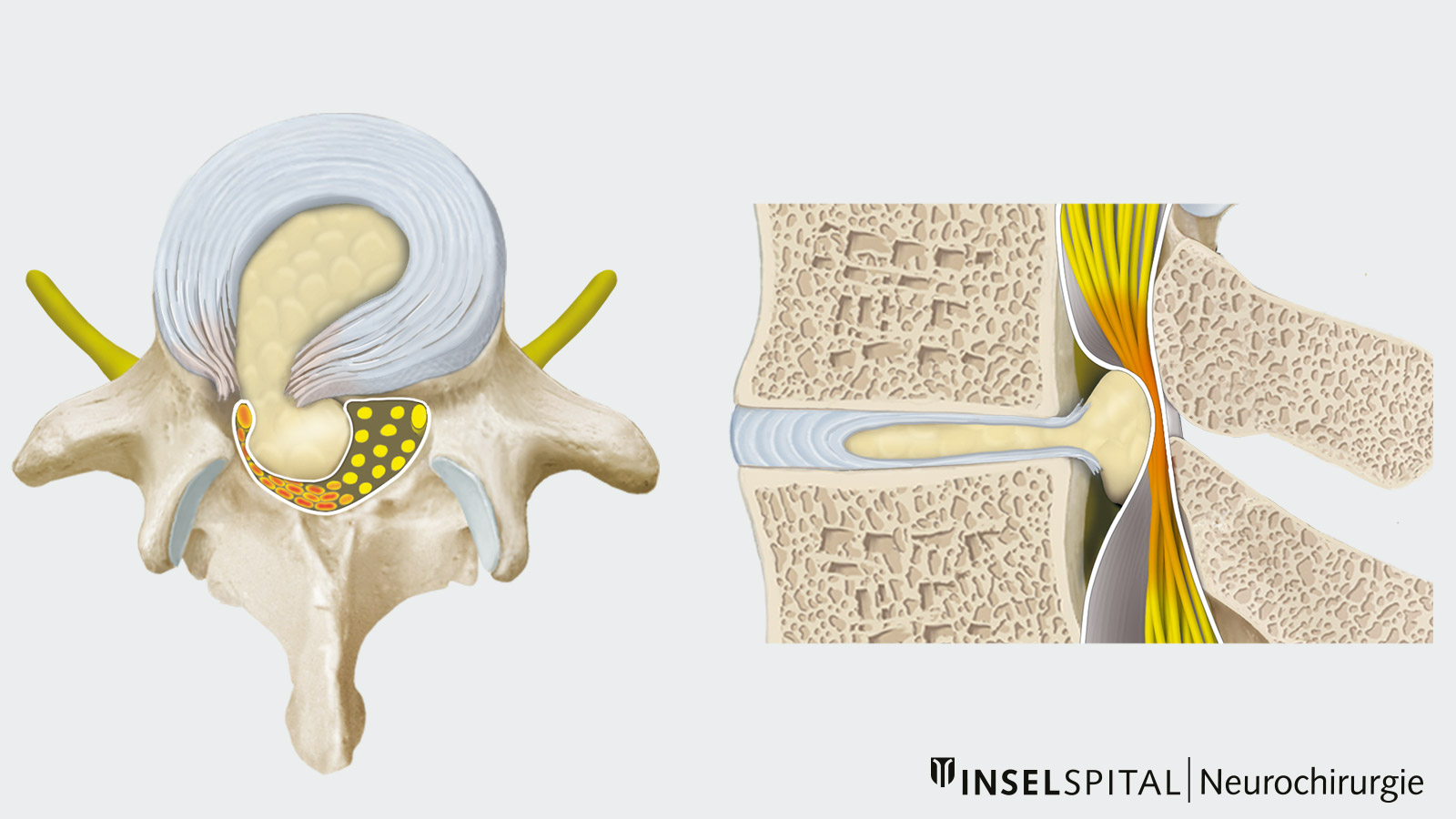
A herniated disc—also known as a slipped disc, disc herniation, or nucleus pulposus prolapse—occurs when tears form in the outer fibrous ring (annulus fibrosus) of the intervertebral disc. This allows tissue from the inner core (nucleus pulposus) to escape toward the spinal canal or nerve roots and compress them.
If the disc tissue remains partially attached to the disc and only a bulge of the annulus fibrosus occurs, this is referred to as a disc protrusion. If, on the other hand, a fragment becomes completely detached from the disc nucleus, this is referred to as a sequestered disc herniation. This detached piece of disc tissue can range in size from a few millimeters to several centimeters.
The herniation becomes clinically significant when nerve roots or the spinal cord are compressed. Depending on the location in the cervical, thoracic, or lumbar spine, different symptoms may result.
There are three typical locations for herniated discs along the spine:
- A cervical herniated disc affects the cervical spine (C-spine)
- A thoracic herniated disc affects the thoracic spine (T-spine)
- A lumbar herniated disc affects the lumbar spine (L-spine)
Herniated discs most commonly occur in the lumbar spine, as this section bears the greatest mechanical load.
When should a herniated disc be operated on?
If surgery is necessary, it is typically performed microsurgically and minimally invasively via a tissue-sparing approach under the surgical microscope or endoscopically. When indicated appropriately, surgical procedures yield good results compared to prolonged conservative therapy. *, *
In most cases of herniated discs, treatment initially involves conservative management in close collaboration with the departments of the Spine Center at Inselspital, particularly Rheumatology and the Pain Center. Symptoms often improve significantly within a few days to weeks with rest, medication, and physical therapy.
Surgical treatment is recommended if symptoms do not improve sufficiently within 6 to 12 weeks or if severe pain, neurological deficits, or loss of muscle strength occur. An acute emergency requiring immediate neurosurgical evaluation exists in cases of complete loss of muscle strength or bladder dysfunction.
If surgery is necessary, it is usually performed microsurgically and minimally invasively via a tissue-sparing approach under the operating microscope or endoscopically. When indicated correctly, surgical procedures show good results compared to prolonged conservative therapy. *, *
There are also more invasive procedures, such as the implantation of an artificial disc or spinal fusion surgery. As a general rule, however, the simplest and least invasive procedure should be chosen first.
Why you should seek treatment at Inselspital
At Inselspital, herniated discs are treated through close collaboration among various medical specialties. The treatment strategy is determined through interdisciplinary collaboration between rheumatology, physical therapy, neurology, neuroradiology, the pain center, and orthopedics. This ensures that every patient receives a personalized and medically optimal treatment plan.
If surgery is necessary, it is typically performed minimally invasively and microsurgically using a tissue-sparing approach under the operating microscope.
Disc surgery is one of the most common neurosurgical procedures at Inselspital.
-
Lurie J, Tosteson T, Tosteson A, Zhao W, Morgan T, Abdu W et al. Surgical Versus Nonoperative Treatment for Lumbar Disc Herniation. Spine. 2014;39(1):3-16.
-
Bailey C, Rasoulinejad P, Taylor D, Sequeira K, Miller T, Watson J et al. Surgery versus Conservative Care for Persistent Sciatica Lasting 4 to 12 Months. New England Journal of Medicine. 2020;382(12):1093-1102.
Further reading
- Adams M, Roughley P. What is Intervertebral Disc Degeneration, and What Causes It?. Spine. 2006;31(18):2151-2161.
- Dowdell J, Erwin M, Choma T, Vaccaro A, Iatridis J, Cho S. Intervertebral Disk Degeneration and Repair. Neurosurgery. 2017;80(3S):S46-S54.
- Miller JAA, Schmatz C, Schultz AB. Lumbar Disc Degeneration. Spine. 1988;13(2):173-178.
- Videman T, Sarna S, Battié M, Koskinen S, Gill K, Paananen H et al. The Long-Term Effects of Physical Loading and Exercise Lifestyles on Back-Related Symptoms, Disability, and Spinal Pathology Among Men. Spine. 1995;20(6):699-709.
