A subarachnoid hemorrhage is a life-threatening emergency that occurs when an aneurysm in the cerebral arteries ruptures. It occurs at a rate of approximately 10 per 100,000 people and mostly affects people between the ages of 40 and 60. The sudden influx of blood into the subarachnoid space causes intracranial pressure to rise rapidly. Typical symptoms include sudden, severe headache, impaired consciousness, and neurological deficits. Immediate treatment is essential.
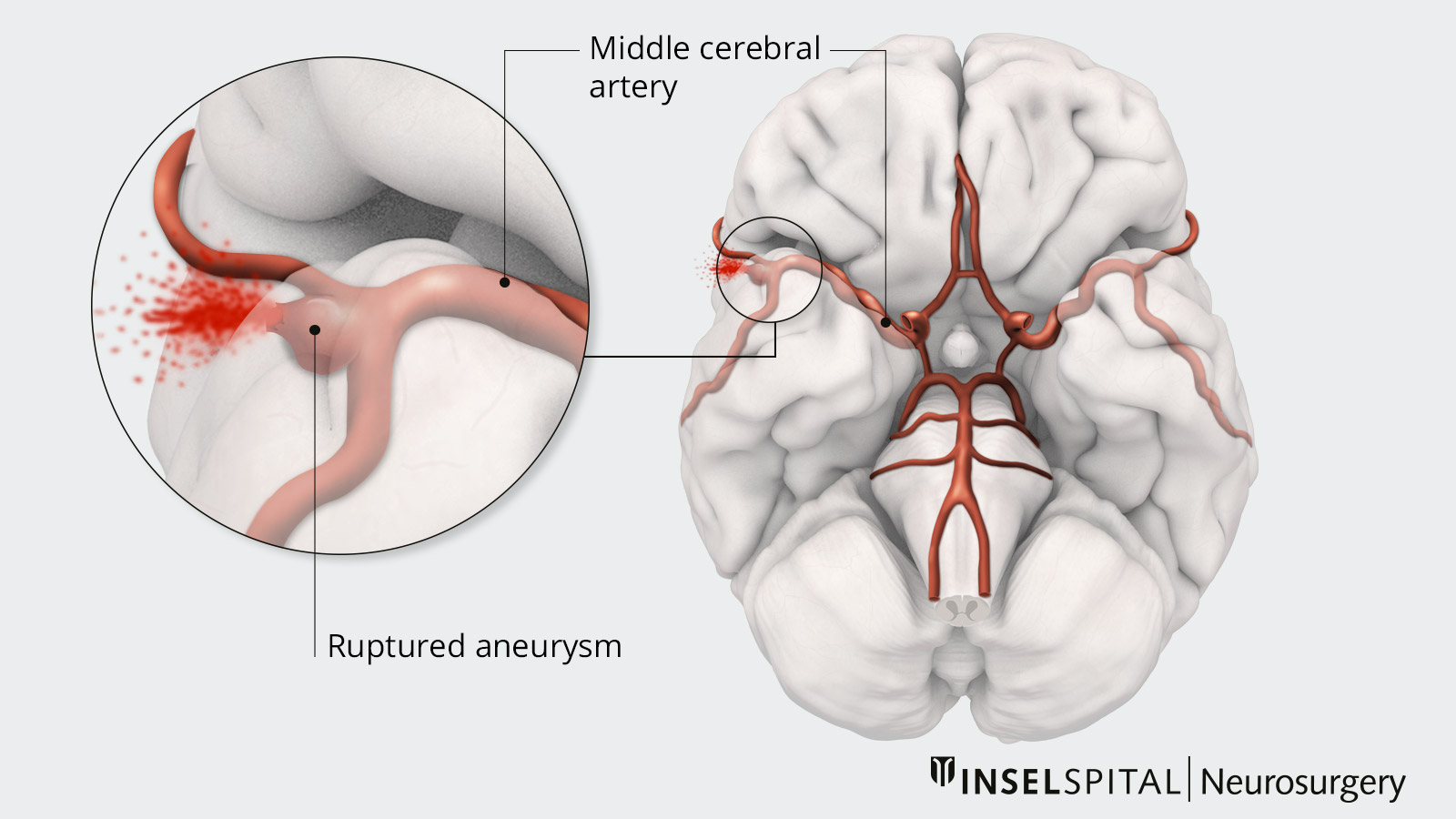
What are the risk factors?
The most important risk factors include high blood pressure, smoking, and excessive alcohol consumption.
Certain connective tissue disorders or vascular abnormalities can also increase the risk.
In rare cases, there is a genetic predisposition, meaning that aneurysms can occur more frequently in certain families.
What are the symptoms of a subarachnoid hemorrhage?
The main symptom is a sudden, severe and extremely painful headache also known as thunderclap headache. The pain can be felt throughout the head and can radiate to the neck and back.
In severe cases, unconsciousness or a seizure may occur only seconds later.
In addition, there may be variable neurological symptoms such as speech disorders, paralysis, sensory disturbances and double vision.
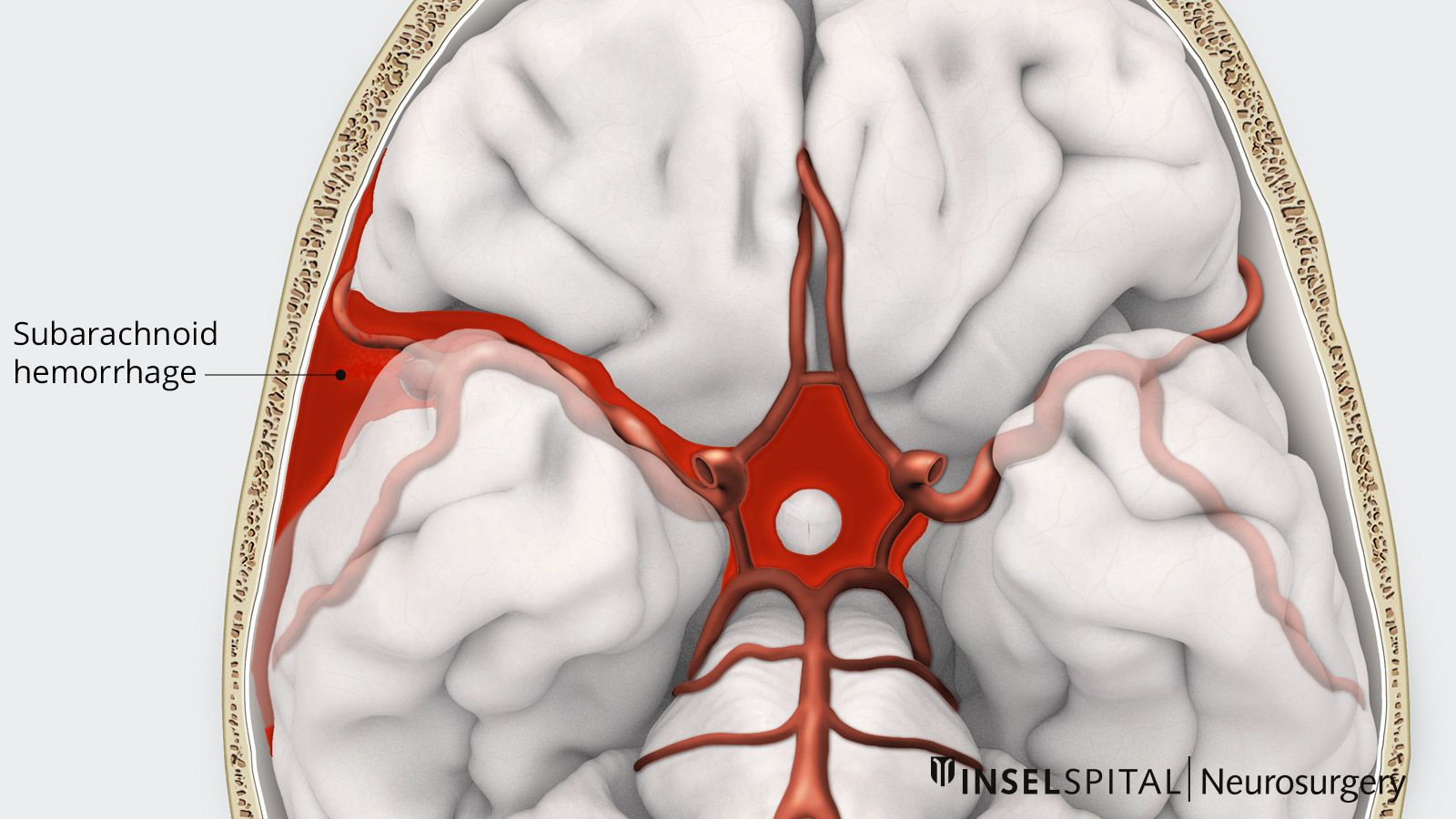
What tests are performed?
Initially, emergency imaging is performed using computed tomography (CT), including vascular imaging, and in rare cases also using magnetic resonance imaging (MRI). In patients with impaired consciousness or intubation, once the diagnosis has been confirmed, external ventricular drainage is often performed to drain cerebrospinal fluid and reduce increased intracranial pressure.
Within 24 hours, a cerebral catheter angiography is performed to precisely locate the site of the bleeding. A specialized interdisciplinary team of neurosurgeons and neuroradiologists then decides on the best treatment method to eliminate the aneurysm and prevent further bleeding – either through endovascular coiling or microsurgical clipping.
In the case of typical symptoms (especially thunderclap headache) or if the Ottawa criteria are met, a lumbar puncture is indicated if a CT or MRI scan was performed more than 6 hours after the onset of symptoms and no evidence of subarachnoid hemorrhage was found. During a lumbar puncture, the cerebrospinal fluid is examined for blood breakdown products that indicate subarachnoid hemorrhage. If the suspicion is confirmed, a catheter angiography is also performed for precise clarification. However, if imaging is performed within the first 6 hours after the onset of symptoms, an additional lumbar puncture is not absolutely necessary due to the high sensitivity of imaging for detecting subarachnoid hemorrhage.
What is the treatment?
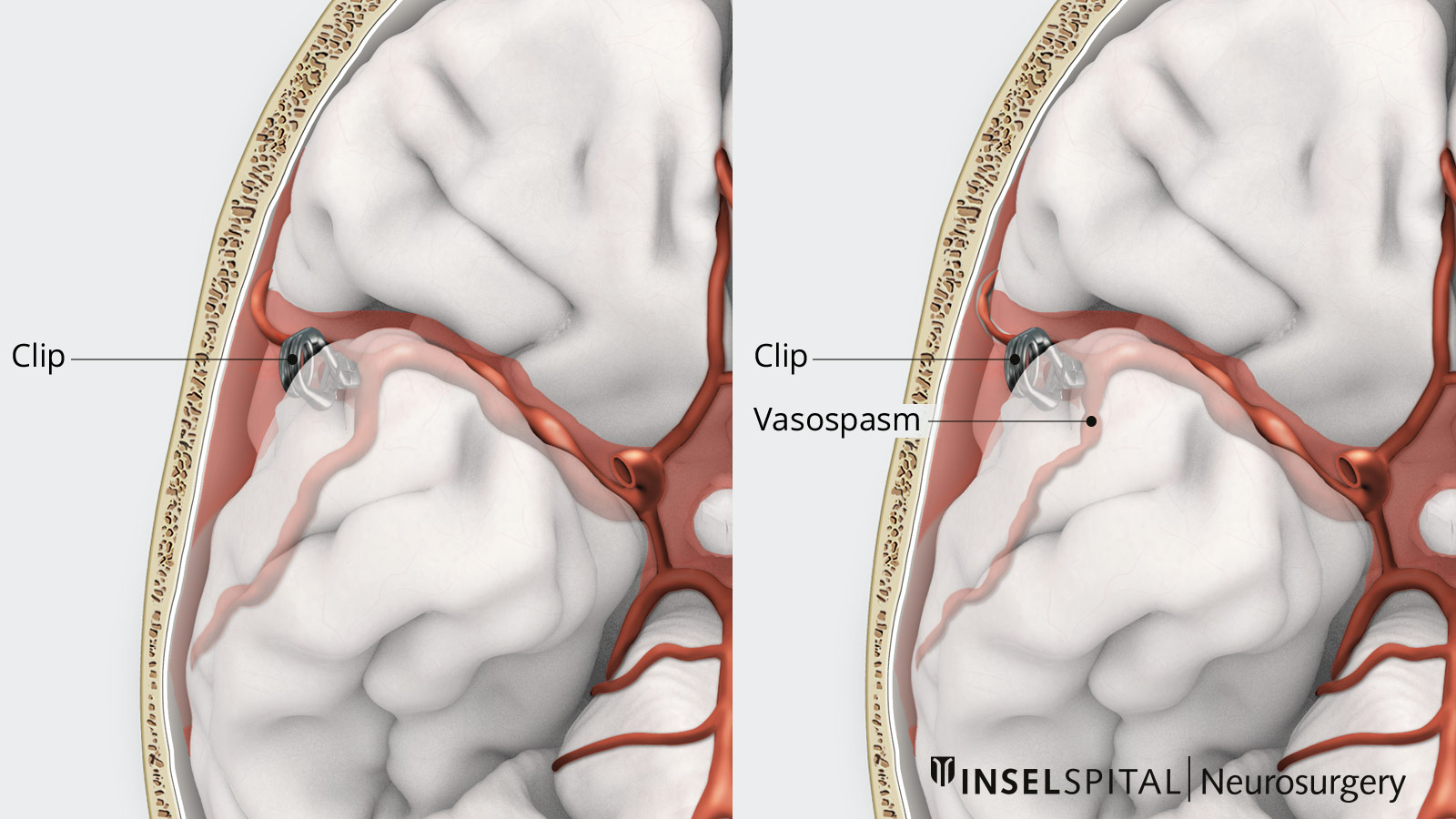
After the aneurysm has been eliminated, close monitoring takes place in the intensive care unit or the neurosurgical-neurological intermediate care unit. The reason for this is that the large cerebral vessels in contact with blood in the subarachnoid space regularly begin to constrict after 3–7 days (vascular spasm or vasospasm). This can lead to circulatory disorders and cerebral infarctions, which occur in about 10–20% of patients.
As a preventive measure, all patients receive the calcium antagonist nimodipine and special monitoring by experienced specialists. Often, there is also a disturbance in cerebrospinal fluid circulation or resorption, which requires external ventricular drainage or lumbar drainage.
If, despite these measures, signs of severe vasospasm or cerebral infarction occur, treatment is carried out according to a step-by-step plan: first, targeted circulatory therapy with induced hypertension and normovolemia. If the symptoms persist, endovascular procedures such as intra-arterial administration of nimodipine or balloon angioplasty are used, or nimodipine is administered into the cerebrospinal fluid.
The vascular spasm usually resolves after about two weeks.
What is the prognosis?
Up to 20% of all subarachnoid hemorrhages are fatal within the first few hours. If the patient survives the hemorrhage, more than half of those affected are still permanently disabled. Rapid diagnosis and treatment are crucial for the prognosis. Patients who have only minor symptoms and are taken to a specialized center immediately usually have a good chance of regaining their abilities almost completely.
Our experience at Inselspital
At Inselspital, patients with subarachnoid hemorrhage are cared for by an interdisciplinary, highly specialized team from the Department of Neurosurgery, neuroradiology, and intensive care medicine. Close cooperation between these disciplines ensures rapid diagnosis, individually tailored treatment, and close follow-up care.
Providing optimal care for patients with aneurysms and researching and treating vascular spasms are among the key focuses of our clinical work and research.
Further reading
- Andereggen L, Beck J, Z’Graggen WJ et al. Feasibility and Safety of Repeat Instant Endovascular Interventions in Patients with Refractory Cerebral Vasospasms. AJNR Am J Neuroradiol. 2017;38:561-567.
- Connolly ES, Rabinstein AA, Carhuapoma JR et al. Guidelines for the management of aneurysmal subarachnoid hemorrhage: a guideline for healthcare professionals from the American Heart Association/american Stroke Association. Stroke. 2012;43:1711-1737.
- Fung C, Inglin F, Murek M et al. Reconsidering the logic of World Federation of Neurosurgical Societies grading in patients with severe subarachnoid hemorrhage. J Neurosurg. 2016;124:299-304.
- Fung C, Balmer M, Murek M et al. Impact of early-onset seizures on grading and outcome in patients with subarachnoid hemorrhage. J Neurosurg. 2015;122:408-413.
- Goldberg J, Schoeni D, Mordasini P et al. Survival and Outcome After Poor-Grade Aneurysmal Subarachnoid Hemorrhage in Elderly Patients. Stroke. 2018;49:2883-2889.
- Hoh BL, Ko NU, Amin-Hanjani S, Chou SH-Y et al. 2023 Guideline for the Management of Patients With Aneurysmal Subarachnoid Hemorrhage: A Guideline From the American Heart Association/American Stroke Association. Stroke. 2023 Jul;54(7):e314-e370.
- Perry JJ, Stiell IG, Sivilotti ML et al. Clinical decision rules to rule out subarachnoid hemorrhage for acute headache. JAMA. 2013 Sep 25;310(12):1248-55.
- van Lieshout JH, Bruland I, Fischer I et al. Increased mortality of patients with aneurysmatic subarachnoid hemorrhage caused by prolonged transport time to a high-volume neurosurgical unit. Am J Emerg Med. 2017;35:45-50.
- Vulcu S, Wagner F, Santos AF et al. Repetitive Computed Tomography Perfusion for Detection of Cerebral Vasospasm-Related Hypoperfusion in Aneurysmal Subarachnoid Hemorrhage. World Neurosurg. 2019;121:e739-e746.
